What causes pelvic organ prolapse, and what are the risk factors (how do I stop it?!)? Pelvic organ prolapse is caused by loss of pelvic support provided by the levator ani muscle, vagina and pelvic connective tissue as well as neurologic injury due to the stretching of the pudendal nerve during childirth. Risk factors include anything causing consistently increased intraabdominal pressure (ie repeated heavy lifting, chronic cough, chronic constipation), increasing age (particularly menopausal status), elevated BMI, Hispanic ethnicity, history of operative vaginal delivery or episiotomy, having had large babies or a large number of babies, and history of previous hysterectomy or other prolapse surgery.
Where does prolapse occur? Apical prolapse occurs as either the uterus or top of the vagina descends toward the vaginal opening. Anterior prolapse occurs along the vagina beneath the bladder, and posterior prolapse happens along the vagina in front of the rectum.
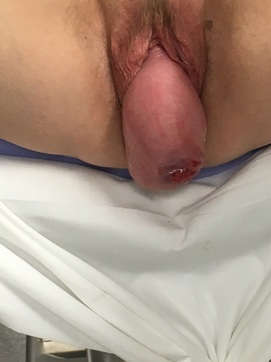
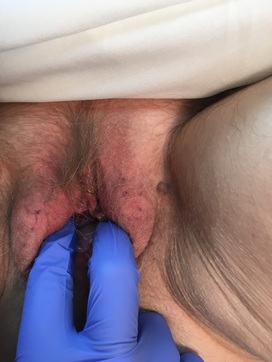
Do I have it?! The most common presenting symptom of pelvic organ prolapse is the feeling of pressure or bulge within the vagina. You probably won’t experience prolapse to the degree in the pictures below (whew!), and mild prolapse, while common, doesn’t necessarily require intervention anyway.
What do I do about it? Again, even though it is common, unless it begins to cause other health issues such is urinary retention/inability to void, recurrent urinary tract infections, kidney damage or difficulty with bowel movements, you aren’t obligated to do anything. I even had a patient with severe prolapse who knit herself a purse to keep her uterus in (seriously!). However, if any of the above issues are present, or your symptoms are affecting your ability to be as active as desired or causing difficulty being intimate with your partner, evaluation is generally advised.
What are treatment options? Other than expectant management, more conservative treatment options include Kegels and vaginal estrogen. Alternatively, another choice may be placement of a pessary (vaginal splint made of rubber), although this does require regular maintenance with removal and cleaning, which are generally done by the patient. Lastly, surgical treatment is often a good option for healthy patients, particularly if they desire to maintain sexual function. Much like a hernia of the abdominal wall, there are several choices of procedure available for treatment of pelvic organ prolapse available. Fortunately, nearly all of these options can be done minimally invasively, which helps the patient get back on her feet faster. Even the patient with severe prolapse below was able to leave the hospital the day after surgery.
So, if you are having any issues with pelvic organ prolapse, be sure to chat with your doctor because you aren’t alone..even if it’s not a topic during your dinner conversations like it is at our house :) (I would like to include a special thanks to our patient who graciously allowed use of the pictures demonstrating a before and after of her prolapse. As she said, “Women need to know about this!”)
Nick
 RSS Feed
RSS Feed